 tidewaterfootandankle@gmail.com
|
tidewaterfootandankle@gmail.com
|
 (757) 497-7575
(757) 497-7575Since 1984, Hampton Roads families and individuals, as well as referring physicians, have counted on Dr. William Grant and his podiatry staff for world-class treatment of foot and ankle problems.
Our patients enjoy:
• Our superior staff. They are personal and they care. It’s not a business to them.
• The most technically advanced podiatry diagnostic equipment in Hampton Roads.
• Our unsurpassed expertise in foot and ankle care.
• The most experienced, technically proficient reconstructive and diabetic foot surgeon in Virginia.
• Our central location, which is easy to get here from anywhere in Hampton Roads.
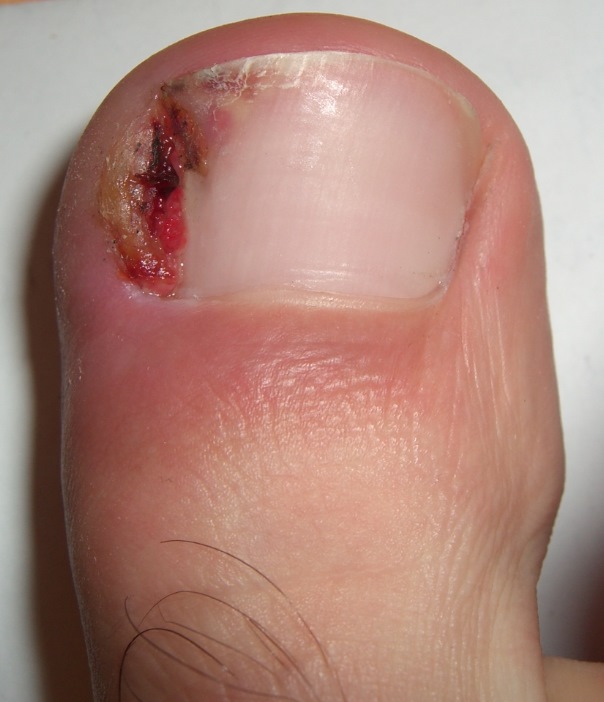
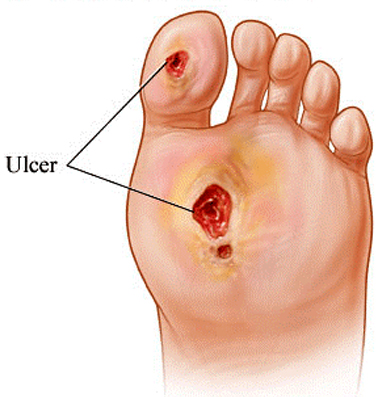
When the toenail grows into the skin next to the nail the skin can also become infected or swollen and the toenail can grow into the swollen skin thus developing an ingrown painful nail. Sometimes this problem is hereditary, other times it is associated with improper trimming of the nail. A common fungus infection which makes the nail very thick and yellow and discolored can also result in that nail becoming ingrown. An ingrown toenail can become infected with redness, swelling, and pain.
Treatment involves removing the offending nail edge. Often this needs to be performed under local anesthetic, which can be painlessly administered at the base of the toe. Before surgery of any kind is performed, a complete history and physical examination is necessary. Special attention to circulation and sensation needs to be addressed before surgery.
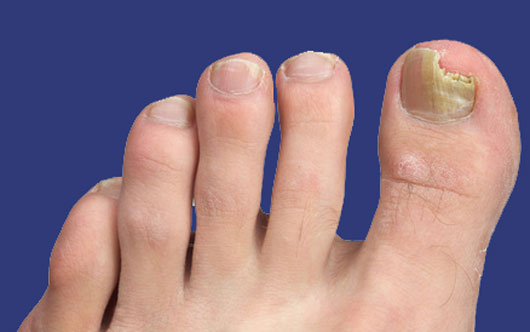
Many patients present with thickened yellow nails, the result of a fungus infection. Disease may also be associated with a chronic fungus infection of the skin of the foot. Once the nail has become fungus infected, it is very difficult to eradicate the fungus, although paint-on topical nail medication is available. However studies have shown its effectiveness to be below 6%. There is 1 prescription medication, Terbinafine, which has a 70%, rate of cure for onychomycosis. This medication can be prescribed and is very safe with proper monitoring. Alternatively, the entire toenail can be safely and surgically removed and the base treated with phenol. The result is no new nail regrowth, however, a false nail forms from the nail bed and the appearance is generally satisfactory.
No matter what the nail condition, the treatment is custom tailored to the patient’s needs and hopes and expectations. These can be discussed at the time of the visit.
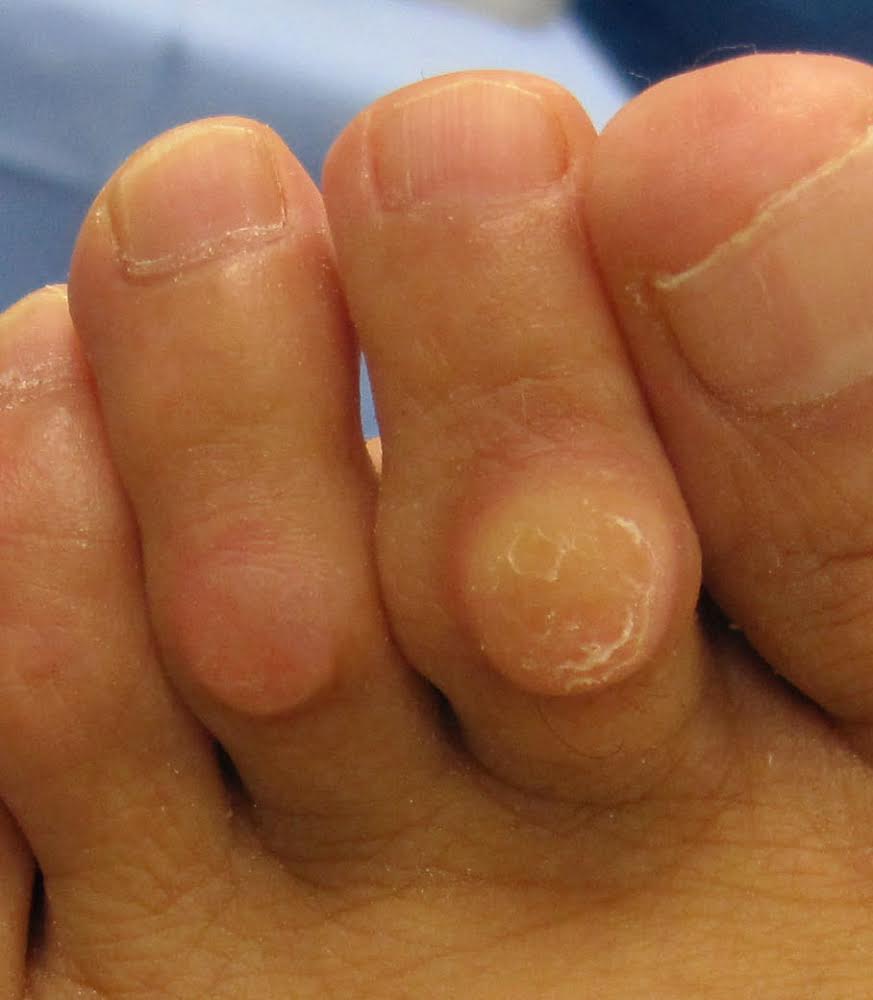
As commonly understood, hammertoes represent a buckling of the toe with a contracted position at either of its 2 joints. A dense hard corn may form at the contracture and this can be painful.
This is a common complaint and develops over time. Causes for hammertoes are many, including, the very high-arched foot, and interestingly, a very flat foot. Both are prone to hammertoe formation, but for entirely different reasons based on the biomechanics of how the foot works. Metabolic diseases including rheumatoid arthritis and diabetes mellitus, can cause the development of hammertoes.
Treatment for hammertoes can begin with the most conservative treatment of all, which is to wear shoes with a wide toe box. Many times a change in footgear makes a material difference in the patient’s discomfort.
If there are painful corns present on the digits, a non-medicated pad from the drugstore may be applied. Medicated pads which claim to reduce the corn associated with the hammertoe need to be avoided. Usually, there is salicylic acid in the medicated pad and it can cause a chemical burn to the skin. This is extremely dangerous in diabetics who have decreased sensation in their feet and for patients who have poor circulation. Since many times people aren’t sure whether sensation or circulation is intact, generally speaking, these medicated pads need to be avoided.
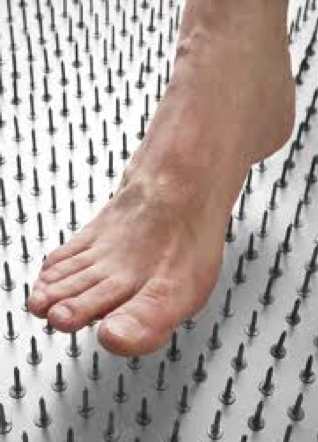
Neuropathy in diabetic patients is a common complaint and increases in frequency of years that people have had diabetes mellitus. Furthermore, poor blood sugar control can make diabetic neuropathy, worse. Patients with diabetic neuropathy frequently complain of #1 numbness; #2, burning or pain; #3, tingling or feeling of pins and needles in the feet. Many people also described their symptoms as feeling like there is a sock bunched up beneath their toes.
For patients who present at the office with complaints of altered sensation or pain in their feet, a full physical examination and medical history are necessary. Sensory testing of the nerves can be preliminarily carried out in the office with simple instruments such as a tuning fork and the filament to test whether feeling is intact. Blood tests can also be ordered, looking at blood sugar control, thyroid function and other markers of potential nerve damage.
Recently, new therapies have become available to decrease the pain and annoying symptoms associated with diabetic neuropathy.
Photo of patients in our practice’s wound center. Each has an ilizarov external fixator in place to help severe wounds or foot deformities heal. Our wound center sees more patients with severe wound or limb salvage or diabetic wounds treated using external fixation than any in our region.
We have pioneered use of external fixation for off loading wounds, published our work in the literature, and are actively involved in its further development.
If you are diabetic or are suffering from heel and foot pain, our foot and ankle specialists can help you. From basic foot and ankle care to advanced surgery, our podiatrists are specifically trained to diagnose, treat and cure these problems: